Those of us living in countries like the U.S., where coronavirus has arrived but not quite exploded exponentially, seem a bit conflicted about what our individual responses should be.
Ideally, we’d simply heed the advice of medical experts at the CDC and WHO instead of politicians who have a vested interest in over-or under-hyping a potential pandemic. But in a heated election season, that appears to be a tall order.
Everyone agrees that we shouldn’t panic (no one responsible would ever tell people to panic), but what does that mean exactly? Is stocking up on food and toilet paper a sign of panic, or a smart precaution? What’s the sweet spot between alarmism and aloofness?
When numbers are still low where you live, it’s easy to say, “Eh, this isn’t that big of a deal.” But the reality is even if you yourself are not at high risk of dying from the virus, millions of people are. And unlike the flu, there’s no vaccine for this. Measures that might seem “extreme” or “panic-driven” are designed to keep spread of the virus to a minimum.
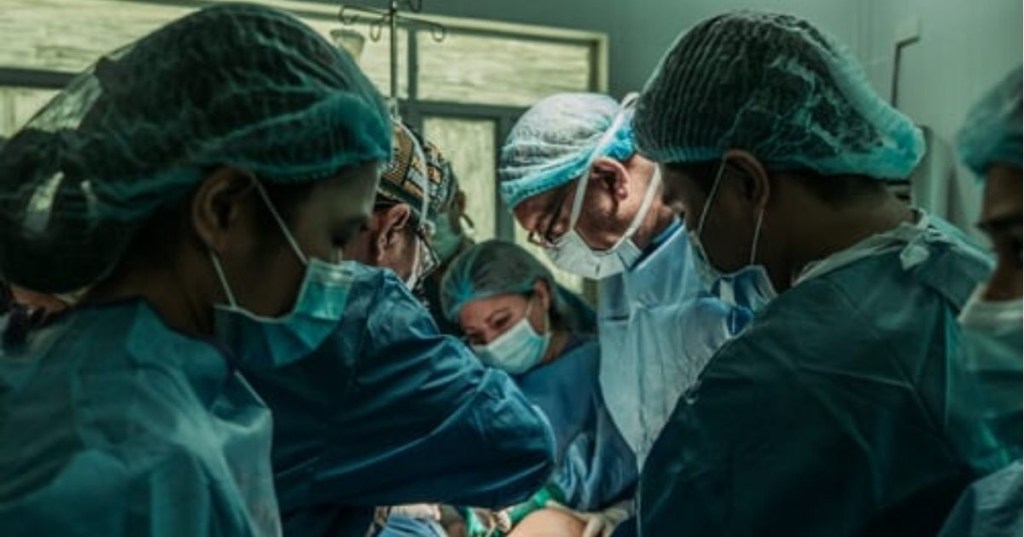
And an ICU physician working in the heart of the outbreak in Italy, Dr. Daniele Macchini, has eloquently explained why limiting the spread is vital.
On February 27, Italy had 650 confirmed cases of COVID-19. Less than two weeks later, they have more than 10,000. The entire country is on lockdown and hospitals are over capacity—a massive contrast to the calm that preceded the storm in the Bergamo hospital where Dr. Macchini works.
Dr. Macchini posted a description on Facebook of what the hospital was like on March 6 vs. what it was like a week before. Below is a condensed translation of his post (which is written in Italian and can be read in its entirety here).
“After much thought about whether and what to write about what is happening to us, I felt that silence was not responsible.
I will therefore try to convey to people far from our reality what we are living in Bergamo in these days of Covid-19 pandemic. I understand the need not to create panic, but when the message of the dangerousness of what is happening does not reach people, I shudder.
I myself watched with some amazement the reorganization of the entire hospital in the past week, when our current enemy was still in the shadows: the wards slowly “emptied”, elective activities were interrupted, intensive care were freed up to create as many beds as possible.
All this rapid transformation brought an atmosphere of silence and surreal emptiness to the corridors of the hospital that we did not yet understand, waiting for a war that was yet to begin and that many (including me) were not so sure would ever come with such ferocity.
I still remember my night call a week ago when I was waiting for the results of a swab. When I think about it, my anxiety over one possible case seems almost ridiculous and unjustified, now that I’ve seen what’s happening. Well, the situation now is dramatic to say the least.
The war has literally exploded and battles are uninterrupted day and night. But now that need for beds has arrived in all its drama. One after the other the departments that had been emptied fill up at an impressive pace. The boards with the names of the patients, of different colours depending on the operating unit, are now all red and instead of surgery you see the diagnosis, which is always the damned same: bilateral interstitial pneumonia.
Now, explain to me which flu virus causes such a rapid drama. And while there are still people who boast of not being afraid by ignoring directions, protesting because their normal routine is”temporarily” put in crisis, the epidemiological disaster is taking place.
And there are no more surgeons, urologists, orthopedists, we are only doctors who suddenly become part of a single team to face this tsunami that has overwhelmed us. Cases are multiplying, they arrive at a rate of 15-20 admissions per day all for the same reason. The results of the swabs now come one after the other: positive, positive, positive. Suddenly the E.R. is collapsing.
Reasons for the access always the same: fever and breathing difficulties, fever and cough, respiratory failure. Radiology reports always the same: bilateral interstitial pneumonia, bilateral interstitial pneumonia, bilateral interstitial pneumonia. All to be hospitalized.
Someone already to be intubated and go to intensive care. For others it’s too late… Every ventilator becomes like gold: those in operating theatres that have now suspended their non-urgent activity become intensive care places that did not exist before.
The staff is exhausted. I saw the tiredness on faces that didn’t know what it was despite the already exhausting workloads they had. I saw a solidarity of all of us, who never failed to go to our internist colleagues to ask “what can I do for you now?”
Doctors who move beds and transfer patients, who administer therapies instead of nurses. Nurses with tears in their eyes because we can’t save everyone, and the vital parameters of several patients at the same time reveal an already marked destiny.
There are no more shifts, no more hours. Social life is suspended for us. We no longer see our families for fear of infecting them. Some of us have already become infected despite the protocols.
Some of our colleagues who are infected also have infected relatives and some of their relatives are already struggling between life and death. So be patient, you can’t go to the theatre, museums or the gym. Try to have pity on the myriad of old people you could exterminate.
We just try to make ourselves useful. You should do the same: we influence the life and death of a few dozen people. You with yours, many more. Please share this message. We must spread the word to prevent what is happening here from happening all over Italy.”
Macchini was speaking to his countrymen, but those of us who live in nations with numbers like Italy had two weeks ago should take note. It’s not just a matter of our own personal risk of critical illness; it’s also about the capacities of our hospitals and the availability of medical personnel. (I live five hours from Seattle, and a nurse friend here told me yesterday that facilities are offering up to $5000 a week for nurses to go work in Seattle right now to help manage the outbreak there. Things are getting real, real quick.)
Italy had 650 cases less than two weeks ago. As of the writing of this article, the U.S. has 755. If we don’t take extreme measures—which many will call mistakenly call “panic”—to keep spread to a minimum, we may soon be facing the same dire straits Dr. Macchini describes in Italy.
Let’s all agree to hunker down at home as much as possible, wash our hands religiously, avoid crowded spaces, stop hoarding medical equipment, and ask that our government be proactive with testing and truthful and transparent about the numbers. And let’s do all of the above without calling any of it “panic.” At this point, it’s not panic, but practicality.