Music, community and joy drive real change
In a small village in Pwani, a district on Tanzania’s coast, a massive dance party is coming to a close. For the past two hours, locals have paraded through the village streets, singing and beating ngombe drums; now, in a large clearing, a woman named Sheilla motions for everyone to sit facing a large projector screen. A film premiere is about to begin.
It’s an unusual way to kick off a film about gender bias, inequality, early marriage, and other barriers that prevent girls from accessing education in Tanzania. But in Pwani and beyond, local organizations supported by Malala Fund and funded by Pura are finding creative, culturally relevant ways like this one to capture people’s interest.
The film ends and Sheilla, the Communications and Partnership Lead for Media for Development and Advocacy (MEDEA), stands in front of the crowd once again, asking the audience to reflect: What did you think about the film? How did it relate to your own experience? What can we learn?
Sheilla explains that, once the community sees the film, “It brings out conversations within themselves, reflective conversations.” The resonance and immediate action create a ripple effect of change.

Across Tanzania, gender-based violence often forces adolescent girls out of the classroom. This and other barriers — including child marriage, poverty, conflict, and discrimination — prevent girls from completing their education around the world.
Sheilla and her team are using film and radio programs to address the challenges girls face in their communities. MEDEA’s ultimate goal is to affirm education as a fundamental right for everyone, and to ensure that every member of a community understands how girls’ education contributes to a stronger whole and how to be an ally for their sisters, daughters, granddaughters, friends, nieces, and girlfriends.
Sheilla’s story is one of many that inspired Heart on Fire, a new fragrance from the Pura x Malala Fund Collection that blends the warm, earthy spices of Tanzania with a playful, joyful twist. Here’s how Pura is using scent as a tool to connect the world and inspire action.
A partnership focused on local impact, on a global mission
Pura, a fragrance company that recognizes education as both freedom and a human right, has partnered with Malala Fund since 2022. In order to defend every girl’s right to access and complete 12 years of education, Malala Fund partners with local organizations in countries where the educational barriers are the greatest. They invest in locally-led solutions because they know that those who are closest to the problems are best equipped to solve and build durable solutions, like MEDEA, which works with communities to challenge discrimination against girls and change beliefs about their education.
But local initiatives can thrive and scale more powerfully with global support, which is why Pura is using their own superpower, the power of scent, to connect people around the world with the women and girls in these local communities.
The Pura x Malala Fund Collection incorporates ingredients naturally found in Tanzania, Nigeria, Pakistan, and Brazil: countries where Malala Fund operates to address systemic education barriers. Eight percent of net revenue from the Pura x Malala Fund Collection will be donated to Malala Fund directly, but beyond financial support, the Collection is also a love letter to each unique community, blending notes like lemon, jasmine, cedarwood, and clove to transport people, ignite their senses, and help them draw inspiration and hope from the global movement for girls’ education. Through scent, people can connect to the courage, joy, and tenacity of girls and local leaders, all while uniting in a shared commitment to education: the belief that supporting girls’ rights in one community benefits all of us, everywhere.
You’ve already met Sheilla. Now see how Naiara and Mama Habiba are building unique solutions to ensure every girl can learn freely and dare to dream.
Naiara Leite is reimagining what’s possible in Brazil
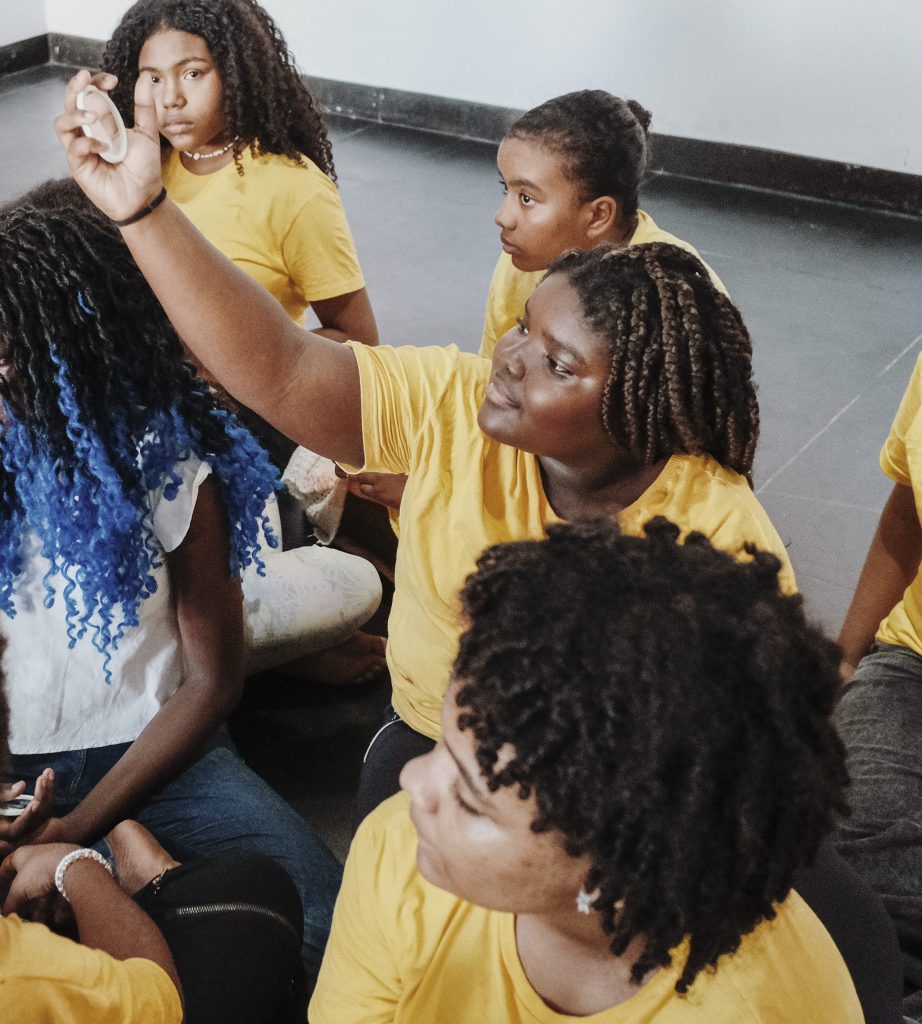
In Brazil, where pear trees and coconut plantations cover the Northeastern Coast, girls like ten-year-old Julia experience a different kind of educational barrier than girls in Tanzania. Too often, racial discrimination contributes to high dropout rates among Black, quilombola and Indigenous girls in the country.
“In the logic of Brazilian society, Black people don’t need to study,” says Naiara Leite, Executive Coordinator of Odara, a women-led organization and Malala Fund partner. Bahia, the state where Odara is based, was once one of the largest slave-receiving territories in the Americas, and because of that history, deeply-ingrained, anti-Black prejudice is still widespread. “Our role and the image constructed around us is one of manual labor,” Naiara says.
But education can change that. In 2020, with assistance from a Malala Fund grant, Odara launched its first initiative for improving school completion rates among Black, quilombola, and Indigenous girls: “Ayomidê Odara”. The young girls mentored under the program, including Julia, are known as the Ayomidês. And like the Pura x Malala Fund Collection’s Brazil: Breath of Courage scent, the Ayomidês are fierce, determined, and bursting with energy.

Ayomidês take part in weekly educational sessions where they explore subjects like education and ethnic-racial relations. The girls are encouraged to find their own voices by producing Instagram lives, social media videos, and by participating in public panels. Already, the Ayomidês are rewriting the narrative on what’s possible for Afro-Brazilian girls to achieve. One of the earliest Ayomidês, a young woman named Debora, is now a communications intern. Another former Ayomidê, Francine, works at UNICEF, helping train the next generation of adolescent leaders. And Julia has already set her sights on becoming a math teacher or a model.
“These are generations of Black women who did not have access to a school,” Naiara says. “These are generations of Black women robbed daily of their dreams. And we’re telling them that they could be the generation in their family to write a new story.”
Mama Habiba is reframing the conversation in Nigeria

In Mama Habiba’s home country of Nigeria, the scents of starfruit, ylang ylang and pineapple, all incorporated into the Pura x Malala Collection’s “Nigeria: Hope for Tomorrow,” can be found throughout the vibrant markets. Like these native scents, Mama Habiba says that the Nigerian girls are also bright and passionate, but too often they are forced to leave school long before their potential fully blooms.
“Some of these schools are very far, and there is an issue of quality, too,” Mama Habiba says. “Most parents find out when their children are in school, the girls are not learning. So why allow them to continue?”
When girls drop out of secondary school, marriage is often the alternative. In Nigeria, one in three girls is married before the age of 18. When this happens, girls are unable to fulfill their potential, and their families and communities lose out on the social, health and economic benefits.
Completing secondary school delays marriage, and according to UNESCO, educated girls become women who raise healthier children, lift their families out of poverty and contribute to more peaceful, resilient communities.

To encourage young girls to stay in school, the Centre for Girls’ Education, a nonprofit in Nigeria founded by Mama Habiba and supported by Malala Fund and Pura, has pioneered an initiative that’s similar to the Ayomidê workshops in Brazil: safe spaces. Here, girls meet regularly to learn literacy, numeracy, and other issues like reproductive health. These safe spaces also provide an opportunity for the girls to role-play and learn to advocate for themselves, develop their self-image, and practice conversations with others about their values, education being one of them. In safe spaces, Mama Habiba says, girls start to understand “who she is, and that she is a girl who has value. She has the right to negotiate with her parents on what she really feels or wants.”
“When girls are educated, they can unlock so many opportunities,” Mama Habiba says. “It will help the economy of the country. It will boost so many opportunities for the country. If they are given the opportunity, I think the sky is not the limit. It is the starting point for every girl.”
From parades, film screenings to safe spaces and educational programs, girls and local leaders are working hard to strengthen the quality, safety and accessibility of education and overcome systemic challenges. They are encouraging courageous behavior and reminding us all that education is freedom.
Experience the Pura x Malala Fund Collection here, and connect with the stories of real girls leading change across the globe.